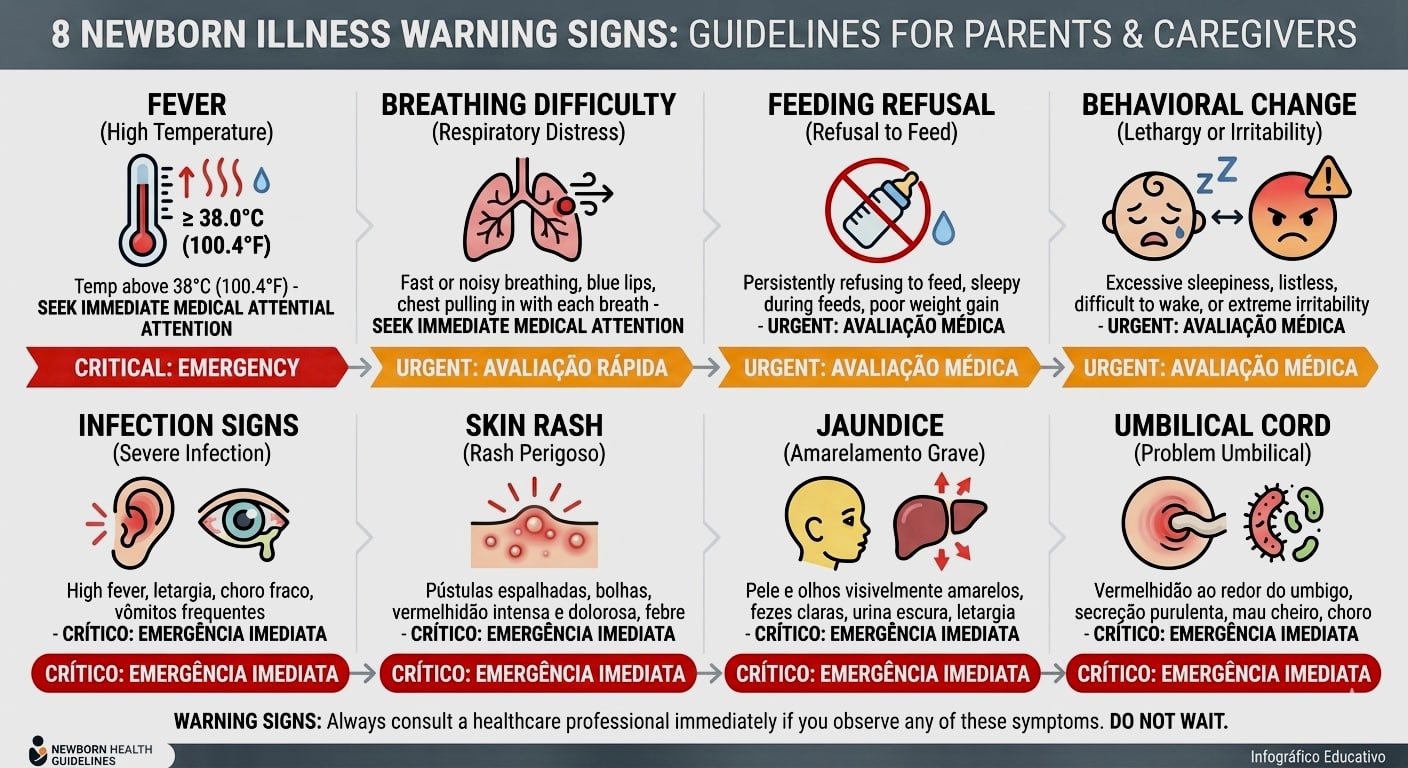
Newborn illness warning signs are among the most critical pieces of knowledge any parent can carry into those first terrifying, beautiful months of caring for a new baby. The problem is that newborns cannot tell you what hurts, cannot describe what feels wrong, and cannot ask for help. Every signal they send comes through behavior, appearance, and physical changes that require an informed, attentive caregiver to interpret correctly.
The stakes could not be higher. What appears to be ordinary fussiness can sometimes be the first sign of a serious bacterial infection. A slight change in feeding patterns can indicate dangerous dehydration. A rash that seems cosmetic can represent a systemic health emergency. Understanding newborn illness warning signs does not mean living in constant fear; it means developing the confident awareness that allows you to act decisively when your baby truly needs medical attention.
This guide covers eight of the most dangerous health threats newborns face during their first months of life, including the symptoms that separate routine discomfort from genuine emergencies, the infections most likely to affect babies in their first weeks, and the prevention strategies that protect developing immune systems from the most serious threats.
Table of Contents
- Understanding Newborn Immune System Vulnerability
- Warning Sign 1: Fever in Newborns
- Warning Sign 2: Breathing Difficulties and Respiratory Distress
- Warning Sign 3: Feeding Refusal and Dehydration
- Warning Sign 4: Extreme Behavioral Changes
- Common Newborn Infections and Prevention Strategies
- Warning Sign 5: Gastrointestinal Symptoms That Signal Danger
- Warning Sign 6: Skin Changes That Require Immediate Attention
- Warning Sign 7: Jaundice Beyond Normal Limits
- Warning Sign 8: Umbilical Cord and Circumcision Site Infections
- When to Call the Doctor for Newborn Illness
- Building Your Newborn Health Monitoring Routine
- Conclusion
- FAQs
Understanding the Newborn Illness Warning Signs Every Parent Must Know
Before examining specific newborn illness warning signs, understanding why newborns are so uniquely vulnerable to illness helps parents appreciate the vigilance this stage requires.
Newborns arrive with immature immune systems that will take months to develop meaningful independent protection. During pregnancy, babies receive maternal antibodies through the placenta, which provide temporary protection against diseases the mother has encountered or been vaccinated against. This passive immunity is real but limited, and it gradually decreases during the first six months of life.
The newborn immune system vulnerability during the first months means that infections capable of causing minor illness in older children or adults can produce life-threatening conditions in very young babies. Bacteria that an older child’s body would contain quickly can spread into a newborn’s bloodstream within hours, causing sepsis. Viruses that produce a mild cold in adults can trigger severe respiratory compromise in a four-week-old infant.
The American Academy of Pediatrics consistently emphasizes that any fever in a baby under three months old is a medical emergency precisely because of this vulnerability. The developing immune system simply cannot mount the same containment response that more mature immune systems can, making rapid escalation far more likely and far more dangerous.
Breastfeeding provides meaningful additional protection during this period, as breast milk delivers maternal antibodies directly to the baby with every feeding. However, even breastfed infants remain significantly more susceptible than older children, and breastfeeding does not eliminate the need for careful health monitoring.
AAP – Signs of Illness in Newborns
1. Fever in Newborns, the Most Urgent Newborn Illness Warning Sign
Newborn illness warning signs vary in urgency, but fever stands alone as the single symptom requiring the most immediate response regardless of any other circumstances.
Any rectal temperature of 100.4 degrees Fahrenheit or 38 degrees Celsius or higher in a baby under three months old requires emergency medical care. This is not a guideline that allows for a wait-and-see approach, and it is not a threshold that becomes less serious because your baby seems to be acting normally. Normal behavior in a baby with a high fever in the first three months does not reduce the medical urgency; it simply means the infection has not yet progressed far enough to affect behavior.
Newborn Immune System Vulnerability in the First Months and Fever Risk
Fever in a newborn indicates the immune system is responding to an invader, but the newborn immune system vulnerability during the first months means that serious bacterial infections, including meningitis, urinary tract infections, bloodstream infections, and pneumonia, can all present initially with fever as their only obvious symptom.
The workup for fever in a newborn typically involves blood tests, urine culture, and sometimes a spinal tap to rule out bacterial meningitis. This process cannot be completed at home and cannot be safely delayed. Bacterial infections in young babies can progress from early-stage infection to serious, life-threatening sepsis within a matter of hours.
Axillary, or underarm, temperature readings are not accurate enough for newborns. Rectal temperature measurement is the clinical standard for this age group. If you do not have a thermometer capable of rectal readings, add one to your newborn care supplies immediately.
Fever Prevention Strategies in Newborns
Limiting exposure to crowded indoor spaces during the first two months significantly reduces transmission risk. Ensuring all household members and visitors are current on their own vaccinations, particularly influenza and pertussis boosters, creates a protective environment. Rigorous hand hygiene before touching the baby remains one of the most effective and underutilized protective measures available.

2. Breathing Difficulties and Respiratory Distress
Breathing changes in newborns represent dangerous newborn health threats that require immediate recognition and response. Newborns breathe faster than older children and adults, typically between 40 and 60 breaths per minute, and their breathing patterns can be irregular with brief pauses of up to ten seconds that are entirely normal.
The newborn illness warning signs that distinguish normal newborn breathing from respiratory distress include breathing rates consistently above 60 breaths per minute, visible retractions where the skin between the ribs or below the ribcage pulls inward with each breath, a grunting sound that accompanies each exhalation, nasal flaring with each breath, and any blue or gray coloring around the lips, fingernails, or fingertips.
Respiratory Syncytial Virus and Newborn Respiratory Risk
RSV is the leading cause of infant hospitalization in the United States and one of the most significant common newborn infections and prevention concerns during the first year of life. In older children and adults, RSV typically produces cold-like symptoms. In newborns, the same virus can cause bronchiolitis, an inflammation of the small airways in the lungs that can rapidly compromise breathing.
For a detailed overview of RSV symptoms, severity indicators, and when to seek emergency care, our dedicated guide on RSV in Babies: 7 Critical Warning Signs Every Parent Must Know provides comprehensive information specifically focused on this infection.
Prevention of respiratory illness in newborns centers on exposure limitation, hand hygiene, and ensuring that anyone with active cold symptoms does not hold or come close to the baby. For high-risk infants, including premature babies and those with underlying heart or lung conditions, pediatricians may recommend additional preventive interventions.

3. Feeding Refusal and Dehydration as Critical Newborn Health Threats
Consistent feeding is how newborns maintain hydration, receive nutrition, and continue gaining weight appropriately. Changes in feeding behavior are therefore significant newborn illness warning signs that parents should monitor carefully.
A newborn who suddenly refuses multiple consecutive feedings, who latches but immediately pulls away repeatedly, or who shows dramatically reduced interest in feeding compared to their established pattern may be signaling an underlying illness. Ear infections, oral thrush, nasal congestion, and systemic illness can all interfere with feeding.
WHO Infant and Young Child Feeding
Recognizing Dehydration in Newborns
Dehydration in newborns escalates more rapidly than in older children because of their smaller total fluid volume and faster metabolic rate. The warning signs include fewer than six wet diapers per day after the first week of life, urine that appears darker yellow rather than pale or clear, a sunken soft spot at the top of the head, dry mouth and lips, absence of tears when crying, and unusual lethargy.
Our detailed resource on Baby Dehydration Signs: How to Recognize and Act Fast covers the complete spectrum of dehydration symptoms and the appropriate response at each level of severity.
Weight monitoring provides an objective measure of adequate feeding and hydration. Most newborns lose up to ten percent of their birth weight in the first few days, then regain it by ten to fourteen days. Failure to regain birth weight by two weeks, or any weight loss after initial regain, warrants immediate pediatric evaluation.

4. Extreme Behavioral Changes in Newborns
Behavioral changes are among the most commonly misread newborn illness warning signs because they require parents to establish a baseline understanding of their individual baby’s normal patterns before recognizing meaningful deviations.
A newborn who becomes suddenly and unusually difficult to wake for feedings, who appears limp or floppy when handled, or who shows a dramatic decrease in movement and responsiveness compared to their normal level of alertness is displaying signs that require immediate medical evaluation. These signs can indicate serious central nervous system involvement, severe infection, or metabolic problems.
Conversely, high-pitched, inconsolable crying that differs distinctly from the baby’s normal cry, particularly when accompanied by other symptoms like fever, poor feeding, or unusual posturing, can also indicate serious illness. Meningitis in newborns can present with a characteristic high-pitched cry that many experienced parents and clinicians describe as distinctly different from hunger or discomfort crying.
Common Newborn Infections and Prevention Strategies
Understanding the most frequently encountered common newborn infections and prevention strategies equips parents with the knowledge to both protect their baby and recognize when an infection has taken hold despite precautions.
Group B Streptococcus
Group B Streptococcus, commonly called GBS, is a bacterial infection that represents one of the most significant infectious risks during the newborn period. Routine GBS screening occurs during pregnancy between 35 and 37 weeks. Mothers who test positive receive intravenous antibiotics during labor to reduce transmission to the baby.
Early-onset GBS disease, which develops within the first week of life, can cause pneumonia, meningitis, and bloodstream infection. The warning signs include respiratory distress, temperature instability, poor feeding, and unusual lethargy. GBS remains a leading cause of serious newborn illness in the United States despite routine screening and prevention protocols.
About Newborn Screening Laboratories
Urinary Tract Infections in Newborns
Urinary tract infections are one of the common newborn infections that parents often overlook because the presenting symptoms, fever, poor feeding, and irritability, are nonspecific and overlap with many other conditions. UTIs are more common in uncircumcised male infants during the newborn period, though they occur across all demographics.
Prompt diaper changing, thorough cleaning during each diaper change, and front-to-back wiping in female infants form the foundation of UTI prevention in this age group. Any unexplained fever in a newborn should prompt urine testing as part of the standard evaluation.
Oral Thrush
Oral thrush, caused by the fungus Candida albicans, presents as white patches on the tongue, inner cheeks, and sometimes the gums of newborns. Unlike milk residue, thrush patches do not wipe away easily. Thrush can make feeding uncomfortable and, if untreated, can spread to the mother’s nipples during breastfeeding, creating a cycle of reinfection.
Prevention includes sterilizing bottle nipples and pacifiers regularly, treating any maternal vaginal yeast infections promptly before delivery, and maintaining good hygiene during breastfeeding. Thrush is treated with antifungal medication prescribed by a pediatrician.
5. Gastrointestinal Symptoms That Signal Danger
Some degree of spitting up, gas, and bowel movement irregularity is entirely normal in newborns. Distinguishing normal gastrointestinal variation from dangerous newborn health threats requires understanding the specific features that elevate concern.
Projectile Vomiting and Pyloric Stenosis
Spitting up is normal; projectile vomiting is not. Projectile vomiting, where formula or breast milk is forcefully expelled in an arc rather than dribbling from the mouth, occurring consistently after feedings and increasing in frequency or force over time, can indicate pyloric stenosis. This condition, where the muscle controlling stomach outflow thickens and blocks normal stomach emptying, typically develops between two and eight weeks of age.
Pyloric stenosis requires surgical correction and, if unrecognized, leads to dangerous dehydration and malnutrition. Any baby demonstrating forceful vomiting after multiple consecutive feedings should be evaluated promptly.
Gastroesophageal Reflux Versus GERD
Most newborns experience gastroesophageal reflux, which is the normal upward movement of stomach contents into the esophagus. True GERD in infants involves reflux that causes poor weight gain, significant feeding aversion, visible discomfort during and after feeding, or respiratory symptoms from aspiration.
Positioning adjustments, including keeping the baby upright for 20 to 30 minutes after feedings and using inclined feeding positions, help manage mild reflux. Severe or persistent symptoms require pediatric evaluation and, in some cases, medication.
Colic: Distressing but Not Dangerous
Colic, defined as crying for more than three hours per day for more than three days per week in an otherwise healthy baby, is one of the most stressful experiences of early parenthood. It is important to distinguish colic from illness-related crying, particularly because colic is a diagnosis of exclusion made only after ruling out underlying medical causes.
If your baby’s crying pattern changes suddenly, if crying is accompanied by fever, changes in feeding, or unusual appearance, or if the crying pattern does not follow the predictable colic pattern of evening intensification and gradual resolution by three to four months, seek medical evaluation rather than attributing the change to colic.
6. Skin Changes That Require Immediate Attention
Newborn skin undergoes significant changes during the first weeks of life, and distinguishing normal variation from the dangerous newborn health threats that can present through skin changes is essential knowledge.
Normal Newborn Skin Conditions
Milia, tiny white bumps across the nose and cheeks, and erythema toxicum, a blotchy red rash with small white centers that appears in the first days of life, are both entirely harmless and require no treatment. Newborn acne, appearing around two to four weeks as small red bumps primarily on the face, is also normal and resolves without intervention. Peeling skin on the hands and feet during the first week is normal, particularly in post-term babies.
Skin Newborn Illness Warning Signs
The skin changes that constitute genuine newborn illness warning signs include any rash accompanied by fever, any spreading redness or warmth around the navel or circumcision site, a purple or red rash that does not fade when pressed, blistering skin, jaundice spreading rapidly down the body, or any rash accompanied by behavioral changes.
For an in-depth examination of the skin conditions that require emergency recognition, our comprehensive resource on 7 Life-Threatening Skin Conditions in Babies Parents Often Miss provides detailed guidance on identification and appropriate response.
7. Jaundice Beyond Normal Limits
Physiological jaundice, the yellowing of skin and eyes caused by elevated bilirubin as the newborn liver adjusts to processing red blood cell breakdown, affects up to 60 percent of full-term newborns and up to 80 percent of premature babies. In most cases, this jaundice appears after the first 24 hours, peaks between days two and four, and resolves within two weeks without treatment.
The newborn illness warning signs related to jaundice that require urgent attention include jaundice appearing within the first 24 hours of life, jaundice spreading below the chest and onto the abdomen and legs, jaundice accompanied by extreme sleepiness and difficulty waking for feeds, dark urine combined with pale stools, and bilirubin levels rising faster than expected on repeat measurements.
Severe untreated jaundice can cause permanent brain damage known as kernicterus. Phototherapy, using specific wavelengths of light to break down bilirubin in the skin, is highly effective when started promptly. Regular visual checks of jaundice progression and bilirubin monitoring per your pediatrician’s schedule are standard parts of newborn care in the first weeks.
8. Umbilical Cord and Circumcision Site Infections
The umbilical cord stump and circumcision site represent two open wound areas that require careful monitoring during the newborn period. Both represent direct pathways for bacterial entry into the newborn body, and infections at these sites can spread rapidly given the newborn immune system vulnerability during the first months.
Umbilical Cord Infection Signs
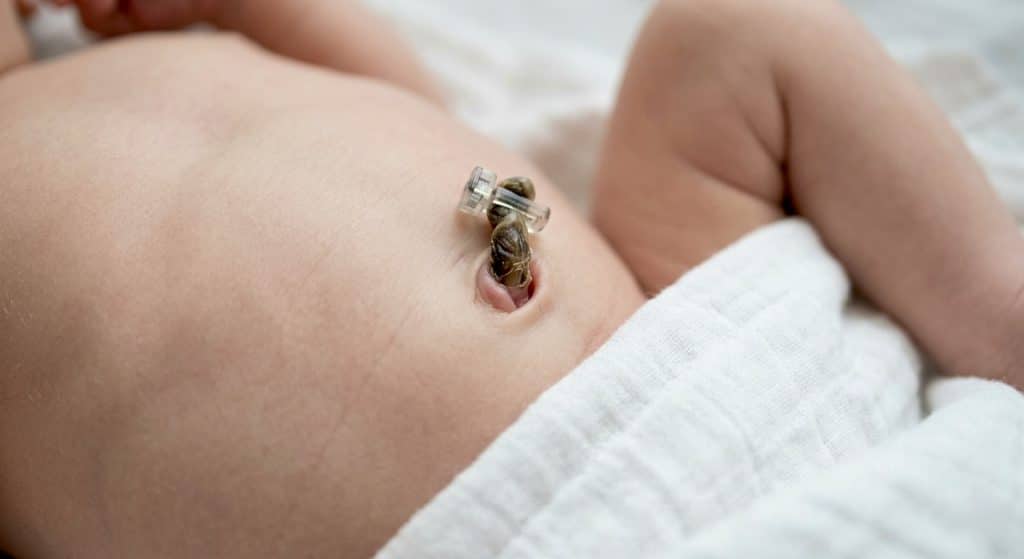
Normal umbilical cord stumps are dark and dry, shrinking and eventually falling off between one and three weeks after birth. Signs of infection at the cord site include redness extending onto the surrounding abdominal skin, warmth or swelling at the base of the cord, any discharge that is not simply a small amount of dried blood or mild wetness, a foul odor, and fever.
Keeping the cord stump clean and dry, folding the diaper waistband below the stump to prevent friction and moisture contact, and avoiding submerging the baby in water until the stump has completely separated and the area has fully healed are the key prevention measures.
Circumcision Site Monitoring
Circumcision healing normally involves some redness, mild swelling, and a yellowish film over the first week. Infection warning signs include spreading redness beyond the circumcision site, significant swelling, bleeding beyond initial healing, fever, and any discharge with an unusual odor. Any of these signs require same-day pediatric evaluation.
When to Call the Doctor for Newborn Illness
Understanding when to call the doctor for newborn illness requires distinguishing between three levels of response: conditions requiring immediate emergency care, conditions requiring urgent same-day evaluation, and conditions appropriate for a scheduled call or next available appointment.
Immediate Emergency Response: Call 911 or Go to the ER
Go directly to the emergency room or call 911 for any of the following: breathing difficulty or significant changes in breathing pattern, blue or gray skin coloring, a seizure or seizure-like activity, extreme difficulty waking the baby, a bulging fontanelle, a high-pitched unusual cry accompanied by other symptoms, any fever of 100.4 degrees Fahrenheit or higher in a baby under three months, and signs of severe dehydration.
For specific guidance on fever emergencies, our detailed post on Baby Fever When to Go to the ER: 7 Critical Warning Signs walks through every fever-related scenario and appropriate response.
Urgent Same-Day Evaluation
Contact your pediatrician immediately for persistent vomiting after multiple consecutive feedings, fewer than six wet diapers in a 24-hour period after day five of life, a rash that is spreading or accompanied by other symptoms, jaundice that appears to be intensifying or spreading, any wound site showing signs of infection, and any behavioral change that seems significant even if you cannot fully describe what seems different.
Trust your instincts. Experienced pediatricians and nurses consistently report that parents who sense something is wrong are right far more often than they are wrong. Your knowledge of your individual baby’s baseline is clinical information that no test can replicate.
Building Your Newborn Health Monitoring Routine
Transforming awareness of newborn illness warning signs into practical daily habits makes monitoring feel natural rather than anxiety-producing. The goal is attentive, confident observation, not hypervigilant surveillance that prevents you from enjoying your baby. Recognizing newborn illness warning signs becomes significantly easier when you build observation into your daily caregiving rhythm rather than treating it as a separate task.
Every feeding, every diaper change, and every moment of skin-to-skin contact is an opportunity to assess your baby’s color, muscle tone, responsiveness, and overall presentation. Parents who understand newborn illness warning signs and integrate this awareness into routine caregiving consistently detect concerning changes earlier than those who rely on scheduled checks alone. The goal is not to monitor anxiously but to observe confidently, knowing that your familiarity with your baby’s normal patterns is your most reliable tool for identifying when newborn illness warning signs are present.
Keep a simple daily log during the first four to six weeks that records feeding times and duration or volume, wet and dirty diaper counts, and any behavioral or appearance changes you notice. This log provides objective information during pediatric appointments and helps you detect gradual trends that might be less obvious when relying on memory alone.
Establish a clear protocol with your pediatrician during the first well visit about their preferred contact method for urgent concerns, their after-hours coverage arrangement, and their specific thresholds for the symptoms most common in newborns. Having these conversations before an emergency makes the decision much clearer when something concerning actually happens.
Our complete resource on Essential Baby Care for New Parents: 7 Vital Secrets provides a broader framework for the daily routines and monitoring habits that support healthy newborn development across all major care areas.
Conclusion
Newborn illness warning signs are not meant to transform parenting into a state of constant medical anxiety. They are meant to transform uncertainty into knowledge, and knowledge into confident, timely action when your baby needs you most.
The eight warning signs covered in this guide represent the health threats most likely to require your fastest response during the first months of your baby’s life. Fever, breathing changes, feeding problems, behavioral shifts, infections, skin changes, jaundice, and wound site infections are all conditions where recognizing the specific features that signal danger can make the difference between early intervention and serious complications.
Your instincts as a parent are a legitimate clinical asset. Every pediatrician who works with newborns knows that parents who sense something is wrong are right more often than not. Trust what you observe, know the warning signs that demand immediate action, and never hesitate to reach out to your pediatrician when something about your baby’s behavior or appearance concerns you.
The investment you make in learning these newborn illness warning signs now is one of the most valuable gifts you can give your child in these irreplaceable first months of life. Every section of this guide returns to the same core principle: newborn illness warning signs are only actionable when parents know what to look for and feel confident enough to act on what they observe.
Looking for comprehensive guidance on caring for your baby? Our book ‘How to Care for Children: From Birth to Age 2’ combines professional nanny experience with evidence based child development research. Written by Kelly and Peter, this guide provides clear, reliable advice rooted in real world childcare. Available in English, Spanish, and Portuguese on Amazon.
Click the link below your preferred language to get your copy!

1. What are the most critical newborn illness warning signs that require emergency care?
The newborn illness warning signs that require calling 911 or going to the emergency room immediately include any fever of 100.4 degrees Fahrenheit or higher in a baby under three months old, significant breathing difficulty including visible chest retractions or persistent grunting, blue or gray coloring around the lips or fingernails, extreme difficulty waking the baby for feedings, a bulging soft spot on the top of the head, and a high-pitched unusual cry. These symptoms indicate conditions that can escalate to life-threatening severity within hours in very young babies, and none of them are safe to monitor at home.
2. How does newborn immune system vulnerability affect illness risk during the first months?
Newborn immune system vulnerability during the first months creates a window where infections that would cause mild illness in older children or adults can cause severe, life-threatening conditions in young babies. Newborns rely primarily on maternal antibodies received through the placenta and breast milk for protection, and their own immune response is too immature to contain rapidly spreading bacterial infections effectively. This is why standard protocols for newborn fever, RSV exposure, and bacterial infections involve more aggressive evaluation and treatment than for older children.
3. What are the most common newborn infections and prevention strategies parents should know?
The common newborn infections and prevention strategies every parent should understand include Group B Streptococcus, which is prevented through prenatal screening and intrapartum antibiotics; RSV, which is prevented through exposure limitation and hand hygiene; urinary tract infections, which are reduced through proper diaper hygiene and prompt changes; and oral thrush, which is prevented by sterilizing feeding equipment and treating maternal yeast infections before delivery. Staying current with recommended vaccinations for all household members creates an additional protective layer around the newborn.
4. When should I call the doctor for newborn illness versus waiting to see how things develop?
Call the doctor for newborn illness without waiting whenever you observe fever in a baby under three months, any breathing changes, more than one episode of forceful vomiting, fewer than six wet diapers per day after day five, jaundice that appears to be intensifying or spreading, any infection signs at wound sites, or any behavioral change that concerns you even if you cannot fully articulate why. The phrase “wait and see” is not appropriate newborn medical guidance. Pediatricians and nurses consistently prefer to evaluate concerns that turn out to be nothing over missing an early presentation of something serious.
5. What are the dangerous newborn health threats related to jaundice that parents often miss?
The dangerous newborn health threats related to jaundice that parents most commonly miss include jaundice appearing within the first 24 hours of life, which is never normal; jaundice spreading rapidly below the chest and onto the legs; extreme sleepiness in a jaundiced baby who is difficult to wake for feedings; and bilirubin levels rising faster than expected between measurements. Severe untreated jaundice causes kernicterus, a form of permanent brain damage. The combination of visible jaundice and any of these accompanying features requires immediate evaluation rather than monitoring at home.
6. How can I tell the difference between normal newborn behavior and newborn illness warning signs?
Distinguishing normal newborn behavior from newborn illness warning signs becomes easier as you learn your individual baby’s specific baseline patterns. Establishing what is normal for your baby in terms of feeding frequency and duration, sleeping patterns, activity level, and cry characteristics during the first weeks gives you a reference point for detecting meaningful deviations. Changes that represent sudden shifts from your baby’s established pattern, symptoms that appear alongside each other rather than in isolation, and any gut feeling that something seems different from your baby’s normal are all reasons to contact your pediatrician without waiting.
7. What role does breastfeeding play in protecting against newborn illness warning signs?
Breastfeeding provides meaningful protection against several of the conditions that produce newborn illness warning signs, primarily through the transfer of maternal antibodies in breast milk. Colostrum, the early milk produced in the first days after birth, is particularly rich in immunoglobulins including secretory IgA, which coats the lining of the infant’s digestive tract and reduces pathogen entry. Breastfed babies generally show lower rates of respiratory infections, gastrointestinal infections, and ear infections compared to formula-fed babies. However, breastfeeding does not create full protection, and breastfed babies require the same careful health monitoring as all newborns.
8. What should I do if I notice newborn illness warning signs in the middle of the night?
If you notice newborn illness warning signs in the middle of the night, your response should be determined entirely by the severity of the symptoms, not by the time of day. Any emergency warning signs including fever in a baby under three months, breathing difficulty, blue coloring, extreme unresponsiveness, or seizures warrant calling 911 or going to the emergency room immediately regardless of the hour. For symptoms that are concerning but not immediately life-threatening, most pediatric practices have after-hours nurse lines specifically designed for exactly this situation. Prepare for these moments in advance by saving your pediatrician’s after-hours contact number and the address of your nearest pediatric emergency facility before you need them.