Knowing the most critical baby dehydration signs is one of the most important skills a parent or caregiver can develop. Babies are among the most vulnerable human beings on the planet when it comes to fluid loss. Their bodies are composed of approximately 75% water at birth, compared to roughly 55% in adults. This difference, combined with an immature kidney system and an inability to communicate thirst, means that dehydration can escalate from a mild inconvenience to a life-threatening emergency within just a few hours.
As a nanny with over ten years of experience working with newborns and infants, I have personally witnessed cases where early recognition of baby dehydration signs made the critical difference between a quick recovery at home and an urgent visit to the emergency room. In this guide, you will find everything you need to identify baby dehydration signs early, understand the causes, take safe action at home, and recognize exactly when your baby needs professional medical care.
Why Babies Dehydrate So Quickly: How to tell if baby is dehydrated?
Before focusing on the specific baby dehydration signs to watch for, it is important to understand why infants are uniquely at risk.
Immature kidneys. A newborn’s kidneys are not fully developed and cannot concentrate urine efficiently until around 12 months of age. This means they lose proportionally more water through urination than an older child or adult would under the same conditions.
High surface-area-to-body-mass ratio. Babies have a relatively large skin surface compared to their total body volume. This causes them to lose water through evaporation at a faster rate, especially during fever or exposure to heat.
Rapid metabolic rate. Infants have higher metabolic demands per pound of body weight than adults. This means they require more fluid relative to their size just to sustain basic bodily functions.
Complete dependence on caregivers. A baby cannot reach for a glass of water when thirsty. They cannot tell you their mouth feels dry or that they have not urinated in hours. Their hydration status depends entirely on the attentiveness of the adults around them.
According to the American Academy of Pediatrics (AAP), even a mild fluid deficit can progress to a medical emergency within hours, particularly during episodes of gastrointestinal illness or exposure to excessive heat. Understanding this timeline is the first step to acting fast.
The Most Common Causes of Dehydration in Infants: Signs of dehydration in babies
Recognizing the circumstances that put your baby at risk is just as important as recognizing the symptoms. The most frequent causes include:
Vomiting and diarrhea. These are the leading causes of dehydration in infants and young children worldwide. A single episode of acute gastroenteritis involving eight or more hours of vomiting or watery stools can cause a fluid deficit equivalent to 5 to 7 percent of body weight in a small infant. According to the National Institutes of Health (NCBI), viruses such as rotavirus and norovirus are responsible for the majority of these episodes in children under two years old.
Fever. For every 1°F rise in body temperature above 99°F, fluid loss through the skin and respiratory tract increases by approximately 10 percent. A baby running a fever of 103°F for several hours is losing significantly more fluid than under normal conditions, making adequate hydration during illness essential.
Baby Fever: What Temperature is Too high
Overheating. Babies dressed in too many layers, placed under stroller covers without ventilation, or left in warm environments without airflow are at serious risk of dehydration through sweating. This risk increases substantially in summer months and during heat waves.
Feeding difficulties. A baby experiencing pain from teething, nasal congestion from a cold, or discomfort from reflux may refuse to nurse or take a bottle. Even a modest reduction in feeding over 12 to 24 hours can create a meaningful fluid deficit in a very young infant.
Illness causing reduced appetite. Any illness that reduces a baby’s willingness to feed, including sore throat, ear infection, or general malaise, can lead to gradual dehydration that parents may not notice until it has already progressed beyond the mild stage.
Read more: 10 Baby Dehydration Signs: How to Recognize and Act Fast?How to Care for a Sick Baby at home
10 Baby Dehydration Signs: From Mild to Severe: Dehydration symptoms in infants
Understanding the full spectrum of baby dehydration signs is essential because the appropriate response depends entirely on the severity of fluid loss. Medical professionals classify dehydration in infants into three levels: mild, moderate, and severe. The 10 baby dehydration signs below are organized from earliest to most critical.
Sign 1. Fewer Wet Diapers Than Usual
This is the earliest and most consistently reliable of all baby dehydration signs. A well-hydrated newborn produces six to eight wet diapers per day. A baby older than one month should have at least four to six. When that count drops noticeably over a 24-hour period, it signals that the baby is not receiving or retaining sufficient fluid.
Here is a simple age-based reference:
| Baby’s Age | Expected Wet Diapers per Day (Normal) | Dehydration Warning |
|---|---|---|
| 0 to 4 days | 1 to 2 (colostrum phase) | 0 wet diapers in 12 hours |
| 5 days to 4 weeks | 6 to 8 | Fewer than 4 per day |
| 1 to 6 months | 4 to 6 | Fewer than 3 per day |
| 6 to 12 months | 4 to 5 | Fewer than 2 per day |
A useful trick for breastfed infants, where output can be harder to judge, is to place a small clean tissue inside the diaper at bedtime. By morning, the tissue will be visibly damp if the baby has urinated. If completely dry, call your pediatrician.
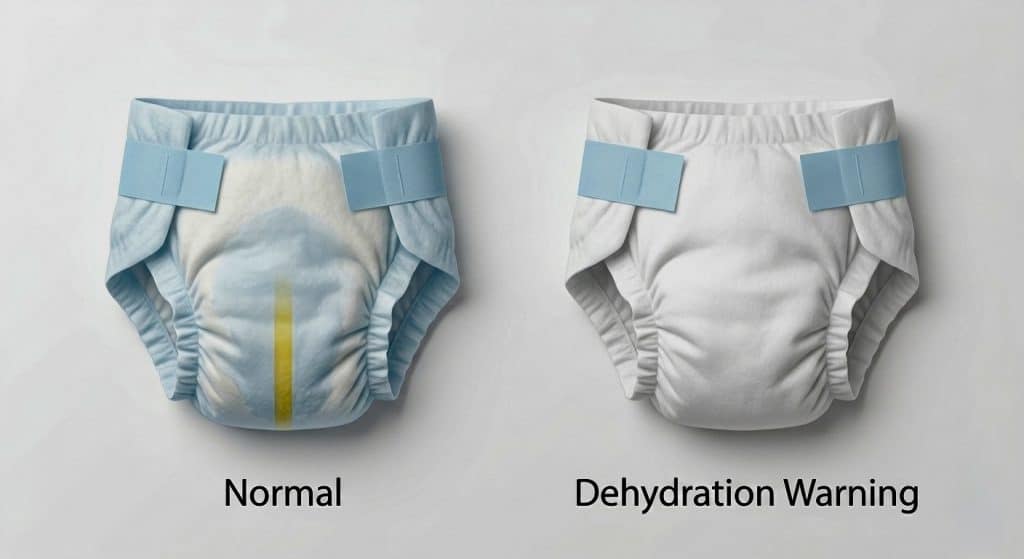
Sign 2. Darker or Stronger-Smelling Urine
A baby dehydration signs is pale yellow to nearly clear urine. Urine that appears deep yellow or amber, or that has a noticeably stronger odor than usual, indicates the kidneys are producing concentrated output as they compensate for reduced fluid intake. A single darker diaper first thing in the morning after an overnight fast is usually normal. Consistently dark urine across multiple diapers throughout the day is a meaningful early warning sign.
Sign 3. Dry or Sticky Mouth and Lips
Run a clean finger along the inside of your baby’s gum line. In a well-hydrated infant, the inner cheeks and gums feel visibly moist and slightly slippery. Early dehydration causes these surfaces to feel tacky or sticky to the touch. The lips may appear slightly chapped or less supple than usual. As dehydration advances, the mouth may produce no saliva whatsoever and feel almost pasty inside.
Sign 4. Crying Without Tears
A well-hydrated baby produces visible tears when crying. A baby in the early stages of dehydration may cry with noticeably fewer tears. At moderate to severe dehydration, crying produces no tears at all. This is one of the most clinically recognized baby dehydration signs and one that pediatricians specifically ask about during phone triage. The complete absence of tears during crying should prompt immediate contact with your pediatrician or a visit to the emergency room.
Sign 5. Decreased Energy and Alertness
A baby who is normally active, alert, and responsive but suddenly seems quieter, less interested in interacting, or less engaged with their surroundings may be in the early stages of dehydration. This change in energy and responsiveness is often one of the first things parents notice before they identify any physical signs. It is important to distinguish this from a naturally quieter temperament or a developmental phase. Dehydration-related lethargy tends to be more pronounced and is almost always accompanied by other physical signs from this list.
Sign 6. Sunken Eyes
Look directly at your baby’s face. With moderate dehydration, the eyes may appear slightly recessed in their sockets, often with a shadowed appearance beneath them. This occurs because the fatty tissue surrounding the eyes contracts when the body is losing fluid. In severe dehydration, the hollowing around the eyes becomes clearly visible without needing to look closely.
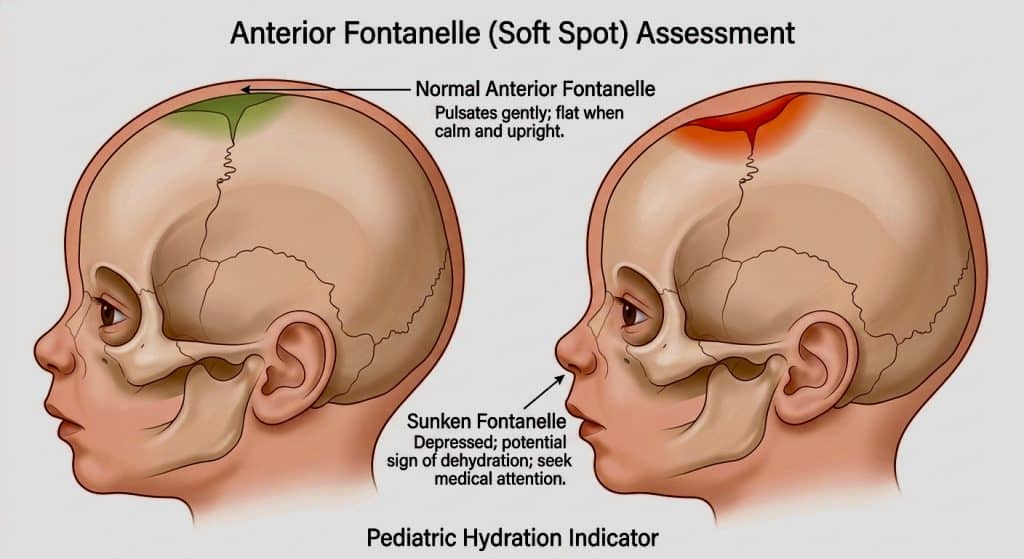
Sign 7. Sunken Anterior Fontanelle (Soft Spot)
The fontanelle is the diamond-shaped soft spot at the top of a baby’s head, where the skull bones have not yet fully fused. In a well-hydrated, resting infant, it appears flat or barely perceptible. With moderate dehydration, it feels noticeably concave or sunken when you gently touch the top of the baby’s skull. This is one of the most reliable clinical baby dehydration signs used by pediatricians during physical examination. Any time you observe a sunken fontanelle alongside other signs in this list, contact your pediatrician immediately.
Sign 8. Poor Skin Turgor (Skin Tenting)
This is a classic clinical test used by pediatricians worldwide. Gently pinch a small fold of skin on the baby’s abdomen or forearm and release it. In a well-hydrated baby, the skin springs back immediately to its original position. With moderate dehydration, the skin returns more slowly, sometimes taking two to three seconds. In severe dehydration, the skin may hold the pinched shape momentarily before returning, a phenomenon called “skin tenting.” The American Academy of Family Physicians (AAFP) identifies abnormal skin turgor as one of the three most useful individual signs for identifying dehydration in children.
Sign 9. Rapid or Labored Breathing
When dehydration is severe enough to reduce circulating blood volume and create a metabolic imbalance, the respiratory system compensates by increasing its rate and depth. A baby breathing noticeably faster than usual, or appearing to be working harder to breathe, in the context of other dehydration signs is showing a serious warning signal. This finding, combined with any of the earlier signs, warrants a call to 911 or an immediate trip to the emergency room.
Sign 10. Extreme Lethargy, Limpness, or Difficulty Waking
A severely dehydrated baby may be extremely difficult to rouse, appear floppy and unresponsive when held, or seem unable to focus or track movement with the eyes. This represents a critical neurological sign indicating that the brain is no longer receiving adequate perfusion. Do not attempt to manage this at home. In the most extreme cases, severe dehydration causes dangerous shifts in blood sodium levels that can trigger seizures or loss of consciousness. If your baby is limp, unresponsive, or having a seizure, call 911 immediately.
Read more: 10 Baby Dehydration Signs: How to Recognize and Act Fast?8 Critical Baby Sleep Problems Parents Always Miss (And What to Do)
Vomiting and Diarrhea: When Baby Dehydration Signs Escalate Fastest – Baby Dehydration treatment at home
Of all the causes covered in this guide, vomiting and diarrhea remain the scenarios where baby dehydration signs escalate most rapidly and unpredictably. Parents often underestimate how quickly a small baby can lose a dangerous amount of fluid during an acute gastrointestinal episode, precisely because each individual vomiting episode or loose stool may not seem alarming on its own.
The problem is cumulative. A baby who vomits four times in three hours and produces three watery stools in the same window may have lost enough fluid to cross from mild into moderate dehydration before the next feeding even begins. This is why monitoring baby dehydration signs continuously during any gastrointestinal illness, rather than reassessing only after each episode, is the safest approach.
What to watch for during a vomiting episode. The color and consistency of vomit carry important clinical information. Vomit that is clear or white and milk-like is generally less concerning. Vomit that is bright green indicates bile and requires immediate medical evaluation, as it may signal an intestinal obstruction. Vomit that is dark brown or contains specks resembling coffee grounds, or that is streaked with blood, is a medical emergency regardless of whether other baby dehydration signs are present.
Managing feeds during vomiting. The most common mistake parents make during a vomiting episode is attempting to offer a full feed immediately after the baby vomits, hoping to replace what was lost. This almost always triggers another vomiting episode, worsening the fluid deficit. The correct approach is to wait 15 to 20 minutes after a vomiting episode, then offer very small volumes, 5 to 10 mL at a time, every five minutes. Slow and steady replacement is far more effective than attempting to compensate with a large volume at once.
When to stop waiting and call. If your baby vomits more than five times within a six-hour period, refuses all fluids for more than two hours, or if any of the baby dehydration signs from the numbered list above appear or worsen between episodes, contact your pediatrician immediately. Do not wait to see if the next feeding stays down before calling.
How to Safely Rehydrate a Dehydrated Baby at Home
Home treatment is appropriate only for mild dehydration in infants older than three months, and always under the guidance or with the prior awareness of your pediatrician. For babies under three months showing any sign of dehydration, contact your pediatrician immediately.
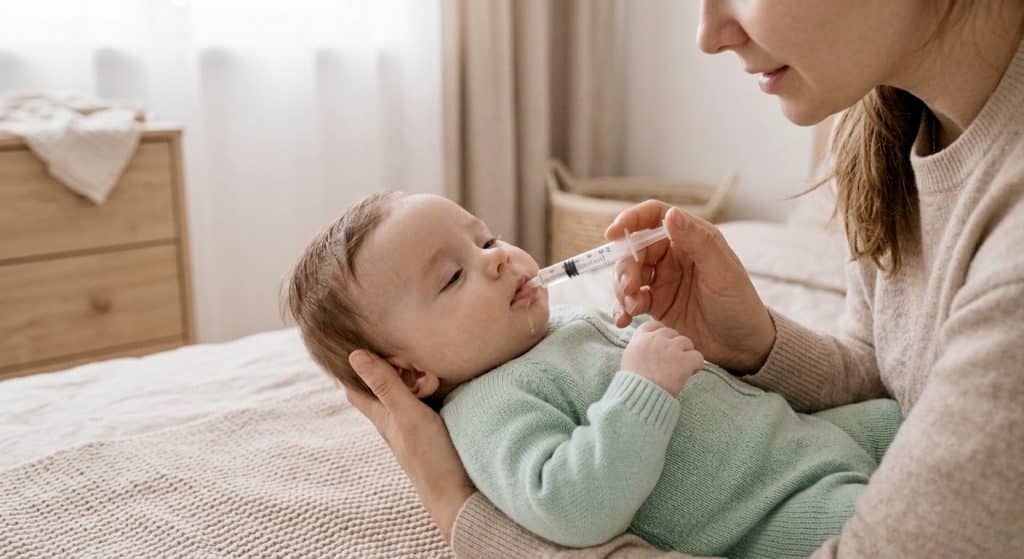
If your baby is breastfed:
Continue nursing on demand and increase the frequency of feeds. Breast milk is approximately 80% water and provides electrolytes, immune factors, and calories simultaneously. Do not restrict breastfeeding during or after an illness. In most cases of mild dehydration in a breastfed infant under six months, returning to more frequent nursing is the most effective and appropriate intervention.
Read more: 10 Baby Dehydration Signs: How to Recognize and Act Fast?Benefits of Continued Breastfeeding During Illness
If your baby is formula-fed (over one month old):
Offer smaller volumes of formula more frequently rather than full feeds at wide intervals. If your baby is vomiting, give very small amounts (5 to 10 mL at a time) every few minutes rather than attempting a full feed at once. Offering a large volume after vomiting frequently triggers another episode, worsening the deficit.
Oral Rehydration Solution (ORS):
For babies older than six months experiencing vomiting or diarrhea, your pediatrician may recommend a commercially prepared oral rehydration solution (ORS) such as Pedialyte, Enfalyte, or a store-brand equivalent. These products are formulated to match the World Health Organization (WHO) specifications for sodium and glucose concentration, making them far more effective at replacing electrolytes than water or diluted juice.
Never offer plain water to infants under six months old. According to the AAP, plain water can dilute sodium levels in a young infant’s blood to dangerous levels, potentially triggering a condition called hyponatremia, which can cause seizures.
Never give sports drinks such as Gatorade or Powerade to babies or toddlers. These products contain far too much sugar and too little sodium to safely rehydrate a small child, and their high sugar content can worsen diarrhea.
Never attempt homemade salt and sugar solutions. The ratio is nearly impossible to replicate correctly at home, and an incorrect concentration can cause more harm than the dehydration itself.
ORS Dosing Guide (for babies under 12 months, per pediatric guidance):
Offer 5 to 10 mL of ORS every five minutes using a small spoon or oral syringe. If the baby tolerates this without vomiting, gradually increase the volume over the following 20 to 30 minutes. The goal during the first two hours is 50 mL per kilogram of body weight for moderate dehydration. Continue breastfeeding or formula-feeding between ORS doses if the baby tolerates it.
When to Call the Doctor Right Away
Contact your pediatrician today (or go to an urgent care clinic) if:
- Your baby is under three months old and shows any baby dehydration sign from the list above.
- Your baby has had no wet diaper in six to eight hours.
- Your baby is crying without producing any tears.
- Your baby has had more than five episodes of vomiting or diarrhea within a 12-hour period.
- Your baby has a fever above 100.4°F (38°C) and is under three months, or above 102°F (38.9°C) at any age.
- Your baby is refusing all feedings, including breastfeeding, for more than four hours.
Call 911 or go to the emergency room immediately if:
- Your baby shows Signs 9 or 10 from the list above.
- Your baby is limp, extremely difficult to wake, or unresponsive.
- Your baby is having a seizure.
- Your baby’s lips or fingernails appear blue or gray.
- Your baby has a deeply sunken fontanelle combined with rapid breathing or heart rate.
- Vomit is bright green, dark brown, or contains blood.
Baby Dehydration Signs by Age: What Changes as Your Baby Grows
Not all baby dehydration signs present the same way across every stage of infancy. Understanding how the signs shift as your baby grows helps you apply the right assessment for the right age, rather than using a one-size-fits-all approach.
Newborns (0 to 4 weeks). In the first days of life, baby dehydration signs can be subtle and are easily confused with normal newborn behavior. The most reliable indicators at this stage are wet diaper count (which should increase by one per day of life in the first week), visible weight loss beyond 7% of birth weight, and a persistently dry mouth. The fontanelle is still quite soft and may be harder to assess accurately. Any concern about dehydration in a newborn requires same-day contact with your pediatrician, without exception.
Young infants (1 to 3 months). Baby dehydration signs in this window become easier to identify because feeding patterns are more established and wet diaper output is more predictable. Reduced diaper count, absence of tears, dry gums, and a noticeably sunken fontanelle are the clearest indicators at this age. Infants in this group are still at very high risk of rapid deterioration and should not be managed at home without explicit pediatric guidance.
Older infants (4 to 6 months). By this stage, many of the classic baby dehydration signs described throughout this article apply fully. The fontanelle is still present and assessable, skin turgor testing is reliable, and tear production is well established. Feeding refusal combined with reduced diaper output over a 12-hour period warrants a pediatrician call.
Infants approaching 12 months (7 to 12 months). As babies begin transitioning to solid foods, monitoring baby dehydration signs becomes slightly more complex. Urine output may vary more with dietary changes. At this stage, behavioral signs such as unusual lethargy, loss of interest in play, and persistent fussiness become more diagnostically useful alongside the physical baby dehydration signs covered in the numbered list above.
Regardless of age, the core principle remains the same: act at the first sign, not the fifth.
Dehydration vs. Normal Variation: What Parents Often Confuse
Reduced feeding during teething. A teething baby may nurse or bottle-feed less enthusiastically for one to three days. This is normal in the absence of other signs. However, if the reduction in feeding extends beyond 24 hours and fewer wet diapers appear, it warrants a call to the pediatrician.
Darker urine in the morning. Most babies produce more concentrated urine first thing in the morning after an overnight fast. A single darker diaper in the morning that resolves with a morning feed is usually not a concern. Consistently dark urine throughout the day is a different matter.
Occasional dry diaper. A single diaper that seems less wet than usual, in an otherwise active, alert, and well-feeding baby, is not a reliable indicator of dehydration. The concern arises when multiple consecutive diapers are dry or only minimally damp.
Quieter than usual. Some babies have naturally quieter temperaments, and developmental stages can temporarily alter activity level. Dehydration-related lethargy tends to be more pronounced and is almost always accompanied by other physical baby dehydration signs.
Preventing Dehydration in Babies: Practical Daily Strategies
Maintain consistent feeding schedules. Breastfed babies under six months should nurse every two to three hours during the day. Formula-fed babies should follow their age-appropriate volume and frequency schedule. During illness or hot weather, increase feeding frequency proactively.
Monitor diaper output as a daily habit. Keeping a simple log of wet diapers, even informally, gives you a reliable baseline. When your baby is ill, a diaper log becomes a clinical tool that your pediatrician will ask about during any phone consultation.
Dress your baby appropriately for the temperature. A general rule for young infants is to dress them in one more layer than you would wear comfortably yourself. During hot weather, one lightweight layer is usually sufficient. Overheating causes evaporative fluid loss through sweating that can accumulate quickly.
Respond promptly to illness. When your baby develops vomiting, diarrhea, or a significant fever, begin offering increased fluids immediately. Do not wait for visible baby dehydration signs to start acting. Early and consistent rehydration prevents most cases from escalating.
Never restrict breastfeeding during illness. Breast milk is the most complete rehydration fluid available for a baby under six months, and it should be offered more frequently during illness, not less.
A Note on Exclusively Breastfed Newborns in the First Week of Life
The first three to five days of life represent a particularly high-risk period for dehydration in exclusively breastfed newborns, especially before the mother’s milk has fully come in. Signs of inadequate intake in a newborn include:
- Fewer than one wet diaper per day of life (one on day one, two on day two, and so forth).
- Visible weight loss exceeding 7 to 10% of birth weight by day five.
- Persistent jaundice.
- A baby who appears inconsolably hungry or, conversely, too sleepy to wake for feeds.
If you are unsure whether your newborn is receiving adequate milk in the first week, contact a lactation consultant and your pediatrician together. Early intervention with feeding support resolves most of these cases without any need for supplementation.

Summary: The 10 Baby Dehydration Signs Action Plan
Recognizing baby dehydration signs early and responding appropriately can prevent a manageable situation from becoming a dangerous one. The 10 baby dehydration signs to keep in mind are: fewer wet diapers, darker urine, dry or sticky mouth, crying without tears, decreased alertness, sunken eyes, sunken fontanelle, poor skin turgor, rapid or labored breathing, and extreme lethargy or limpness. Here is a quick reference of the key action steps:
- Know the baseline. Track your baby’s normal wet diaper count, urine color, and feeding patterns so that any deviation is immediately obvious.
- Act at the first mild signs. Do not wait for the baby to appear severely ill. Begin increasing feeding frequency and monitoring closely at Sign 1 or Sign 2.
- Follow AAP guidelines. Use breast milk or formula for babies under six months, and consult your pediatrician before introducing ORS.
- Never give plain water to babies under six months, sports drinks, or homemade salt solutions.
- Call your pediatrician when in doubt, especially if your baby is under three months old.
- Call 911 or go to the ER immediately for Signs 9 or 10, seizure, limpness, or inability to wake the baby.
I would like to emphasize that the parents and caregivers who prevent emergencies are those who constantly observe their babies and act quickly. Dehydration is one of the most preventable serious health problems in childhood. With the right knowledge and habits, you are already the best protection for your baby.
Read more: 10 Baby Dehydration Signs: How to Recognize and Act Fast?Looking for comprehensive guidance on caring for your baby? Our book ‘How to Care for Children: From Birth to Age 2’ combines professional nanny experience with evidence based child development research. Written by Kelly and Peter, this guide provides clear, reliable advice rooted in real world childcare. Available in English, Spanish, and Portuguese on Amazon.
Click the link below your preferred language to get your copy!

1. What is the first sign of dehydration in a baby?
The earliest and most consistently reliable sign is a reduction in wet diapers. A well-hydrated baby produces four to eight wet diapers per day depending on age. When that number drops noticeably, it is an early signal that the baby is not receiving or retaining sufficient fluid. Simultaneously, the urine may appear darker yellow and have a stronger odor than usual. Dry or sticky gums are another early baby dehydration sign that often appears at the same time. Checking both diaper output and gum moisture together gives you a much more accurate picture than relying on either alone.
2. Can a breastfed baby become dehydrated even if nursing frequently?
Yes, though it is less common than in formula-fed infants. A breastfed baby can become dehydrated if the mother’s milk supply is insufficient, if the baby is not latching effectively and therefore not transferring milk adequately, or if the baby is too ill or fatigued to nurse effectively. If you are concerned, a weight check at your pediatrician’s office will provide a clear picture. It is also worth knowing that baby dehydration signs in breastfed newborns during the first week of life can be more difficult to detect because feeding cues and output patterns are still being established.
When in doubt, request a weighted feed assessment at your pediatrician’s office or with a certified lactation consultant.
3. How quickly can a baby become dehydrated?
Very quickly. In a small infant under three months old, significant fluid loss through repeated vomiting or diarrhea can create a measurable deficit within four to six hours. This is why prompt action at the first baby dehydration sign is essential, rather than waiting to see how the day unfolds. Many parents make the mistake of assuming that because their baby nursed an hour ago, dehydration is not yet a concern. In reality, ongoing losses from diarrhea or fever can outpace intake even during active feeding.
Monitoring baby dehydration signs continuously during any illness episode, rather than checking once and reassuring yourself, is the safest approach.
4. Is Pedialyte safe for babies under six months?
The AAP recommends consulting your pediatrician before giving any ORS, including Pedialyte, to an infant under six months. For the youngest babies, continued breastfeeding is almost always the preferred first-line approach. That said, if your pediatrician does recommend an ORS for a younger infant based on clinical assessment, follow their specific dosing instructions carefully.
Never substitute a sports drink or homemade solution because you cannot access Pedialyte. Recognizing baby dehydration signs early enough to act while breastfeeding is still effective is the best way to avoid needing ORS altogether in this age group.
5. Can overheating cause dehydration in a baby who is feeding normally?
Yes. When a baby is exposed to a warm environment, fluid losses through sweating and evaporation increase significantly, sometimes outpacing their normal intake. During heat waves or in poorly ventilated spaces, increasing feed frequency is a reasonable preventive measure. What makes heat-related cases particularly tricky is that baby dehydration signs from overheating can develop without any illness, vomiting, or diarrhea, so parents are sometimes caught off guard.
A baby who seems slightly flushed, less active than usual, or who has produced fewer wet diapers on a hot day is showing early baby dehydration signs that deserve immediate attention, even if they appear otherwise well.
6. What is the sunken fontanelle and why does it matter?
The anterior fontanelle is the diamond-shaped soft area on the top of a baby’s head, where the skull bones have not yet fully fused. In a hydrated baby at rest, it appears flat. A sunken or concave fontanelle indicates that the tissues surrounding it have contracted due to fluid loss. It is one of the more reliable clinical baby dehydration signs and should prompt an immediate call to the pediatrician if accompanied by other signs from this list.
7. Can I use baby dehydration signs to decide whether to go to the ER or wait?
Yes. The 10 baby dehydration signs in this guide are organized precisely for that purpose. Signs 1 through 5 (fewer wet diapers, darker urine, dry mouth, crying without tears, and decreased alertness) indicate mild to early moderate dehydration, where a pediatrician call and home monitoring are appropriate first steps. Signs 6 through 8 (sunken eyes, sunken fontanelle, poor skin turgor) indicate moderate dehydration that requires same-day medical evaluation. Signs 9 and 10 (rapid breathing and extreme lethargy or limpness) are emergency signals. Call 911 or go to the ER immediately if you observe either of those two baby dehydration signs.
8. Are baby dehydration signs different during a heat wave versus during illness?
The physical baby dehydration signs themselves are the same regardless of cause. However, heat-related dehydration tends to develop more gradually and may initially present only as reduced urine output and unusual fussiness, without the vomiting or diarrhea that often accompanies illness-related cases. During a heat wave, parents sometimes miss early baby dehydration signs because the baby is not visibly sick. Monitoring wet diapers and offering extra feeds during hot weather, even when your baby appears well, is the most effective prevention strategy.
9. What is the fastest way to confirm baby dehydration signs at home before calling the doctor?
The fastest three-step check combines the most reliable baby dehydration signs into a 60-second assessment. First, count the wet diapers from the past six to eight hours. Second, run a clean finger along the inside of the gum line to check for moisture. Third, gently pinch a fold of skin on the abdomen and observe how quickly it returns to normal. If two or three of those checks produce abnormal results, you are looking at confirmed baby dehydration signs that warrant an immediate call to your pediatrician. Having this three-step routine in mind means you are never guessing when it matters most.
10. How do I track baby dehydration signs if my baby is in daycare?
Ask your daycare provider to log wet diaper changes throughout the day, noting approximate volume and color whenever possible. Most licensed childcare providers are trained to recognize basic baby dehydration signs and should alert you immediately if output drops significantly or if the baby appears unusually lethargic or refuses feeds. When your baby is ill, request more frequent updates and, if possible, bring them home so you can monitor baby dehydration signs directly throughout the day.
Sources and References
- American Academy of Pediatrics (AAP). Signs of Dehydration in Infants and Children. HealthyChildren.org.
- National Institutes of Health (NIH), NCBI. Pediatric Dehydration, StatPearls. Last updated June 2024.
- American Academy of Family Physicians (AAFP). Diagnosis and Management of Dehydration in Children.
- Nationwide Children’s Hospital. Dehydration: Overview and Hydration Recommendations.
- Merck Manual Professional Edition. Dehydration in Children.
- Lurie Children’s Hospital. Dehydration in Kids: Signs and Treatment.




